Superspeciality treatment often involves multiple experts, complex decisions, and tight timelines, where gaps can cost outcomes. Case coordination ensures all specialists, diagnostics, and therapies stay aligned through a single, structured care pathway.
It reduces delays, prevents miscommunication, and ensures consistent treatment decisions, making complex care safer, faster, and more effective for patients.
Kasturi Medical Centre, a standout superspeciality hospital in Joka, brings structured coordination into every treatment journey.
Today’s blog explains how case coordination makes complex treatment safer, faster, and more reassuring for patients.
Why superspeciality care breaks without coordination
Superspeciality care breaks without coordination because multiple specialists work in silos, leading to fragmented decisions, delayed interventions, duplicated tests, and critical communication gaps that compromise treatment accuracy and patient outcomes.
That is why case coordination in hospitals has become essential rather than optional.
Too many specialists, too many handoffs, too little shared context
Each specialist sees only part of the story. A cardiologist focuses on the heart. An oncologist studies tumour behaviour. A neurologist evaluates brain signals.
Too many specialists and frequent handoffs without shared context lead to
- Reports get repeated
- Critical findings are delayed
- Patients become messengers between doctors
The real-world cost: delays, duplicate tests, missed follow-ups, and avoidable complications
| Problem | What Happens | Patient Impact |
| Duplicate diagnostics | Tests repeated unnecessarily | Extra cost and delay |
| Missed follow-ups | Treatment gaps | Disease progression |
| Communication errors | Medication overlap | Safety risks |
Case coordination vs care coordination vs case management (quick clarity)
These terms sound similar but serve different roles.
What each term usually means in hospitals
- Care coordination for superspeciality treatment ensures services connect smoothly.
- Case coordination manages active treatment sequencing.
- Case management monitors long-term recovery and compliance.
Where the “case coordinator” sits in the care team
A patient care coordinator in a hospital works between departments. They are not replacing doctors. They connect them.
They communicate with:
- Consultants
- Nursing teams
- Diagnostics
- Insurance desks
- Families
The clinical case manager’s role in the hospital ensures decisions translate into action.
The Daily Responsibilities of a Case Coordinator

Case coordinators organise appointments, ensure reports are ready, align specialist communication, guide families through timelines, and monitor treatment progress to prevent delays or errors.
Appointment + diagnostics sequencing (the domino logic)
Tests must happen in the right order. Wrong sequencing wastes days.
- MRI before surgery planning
- Biopsy before chemotherapy
- Cardiac clearance before major operations
Records and report readiness
Missing records delay critical decisions, so coordinators ensure all reports are ready, imaging films are available, labs are complete, and prior medical history is organised before treatment planning begins.
Cross-department communication
Cross-department communication ensures all teams stay aligned in real time, reducing miscommunication, avoiding delays, and keeping treatment decisions consistent across specialities.
Family guidance + expectation setting
Family guidance and expectation-setting ensure that patients and caregivers understand the treatment plan, timelines, risks, and outcomes.
This is where patient navigation services in hospital programs reduce anxiety, prevent confusion, and improve overall compliance with care.
How coordination shapes the treatment plan in superspeciality cases
Case coordination supports multidisciplinary treatment planning by ensuring specialists review shared data together. Collaborative decisions improve accuracy, reduce bias, and personalise treatment strategies.
MDT planning and why it improves plan quality
A multidisciplinary team treatment plan (MDT) brings experts together before treatment begins.
Who’s in the MDT (Multidisciplinary Team)
Depending on the condition:
- Surgeons
- Oncologists
- Cardiologists
- Neurologists
- Radiologists
- Pathologists
This improves coordination of treatment plans across oncology, cardiology, and neurology departments.
How MDTs reduce tunnel vision
MDTs ask:
- Is surgery best?
- Can radiation work?
- Is medication safer?
A structured MDT culture is a defining feature of Kasturi Medical Centre, a revered superspeciality hospital in Joka, focused on outcomes rather than speed alone.
The Structured “Coordination Workflow” That Prevents Delays and Errors
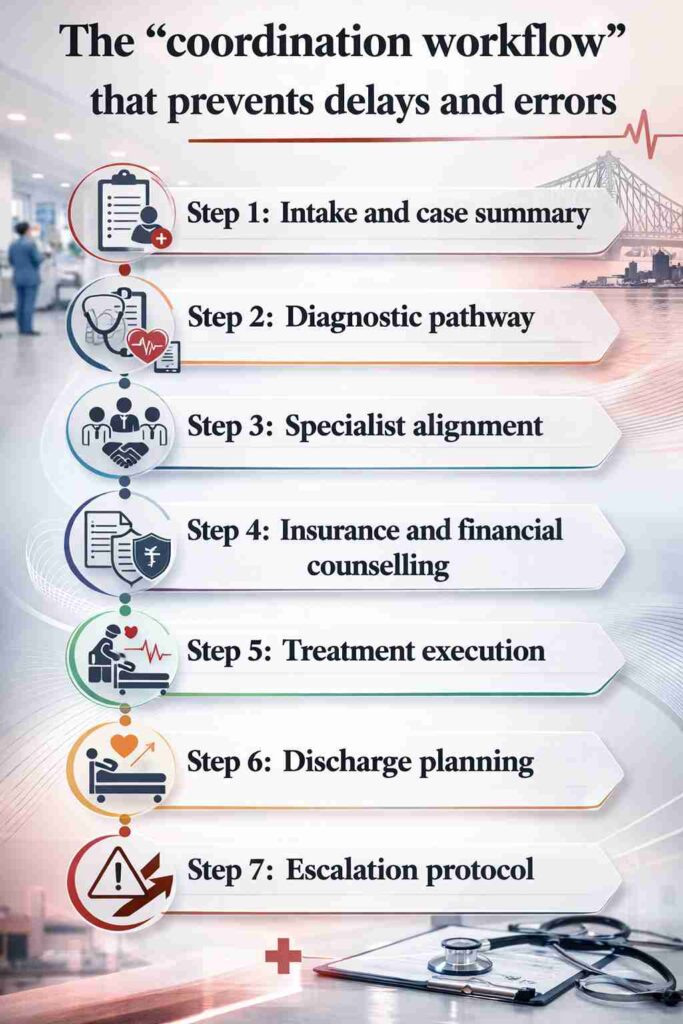
Structured coordination workflows standardise intake assessment, diagnostics, specialist consensus, financial approvals, treatment execution, discharge planning, and escalation monitoring to reduce preventable delays and complications.
Step 1: Intake and case summary
A concise one-page clinical summary captures diagnosis, history, and priorities. Every specialist understands the patient quickly before decisions begin.
Step 2: Diagnostic pathway
Tests are sequenced logically to avoid repetition and delay. The right investigation happens at the right time for accurate planning.
Step 3: Specialist alignment
Consultants review findings together before treatment starts. Shared agreement prevents conflicting opinions and unnecessary changes later.
Step 4: Insurance and financial counselling
A structured TPA insurance coordination hospital ensures timely admission, smoother billing, and uninterrupted treatment without financial or administrative delays.
Step 5: Treatment execution
Treatment execution ensures everything is in place before intervention, with
- OT scheduling confirmed
- Medications prepared
- And ICU availability secured
All this helps prevent last-minute delays and maintain continuity of care.
Step 6: Discharge planning
Discharge planning and follow-up coordination reduce complications and prevent avoidable readmissions.
Step 7: Escalation protocol
Patients receive clear instructions for warning symptoms after treatment. Knowing whom to contact ensures a faster response during emergencies or recovery concerns.
Where case coordination matters most (superspeciality examples)
Case coordination matters most in superspeciality care where multiple departments intersect, ensuring complex treatments stay aligned, timelines are met, and critical decisions are executed without delays or communication gaps.
Oncology
Biopsy, staging, MDT review, and treatment sequencing must follow a precise order. Without coordination, critical weeks can be lost before therapy even begins.
Cardiology
Imaging findings guide cath lab decisions and determine whether a stent or bypass is safer. Timely coordination prevents dangerous delays in heart care.
Neurosciences
Stroke management depends on rapid handoffs between emergency, imaging, and intervention teams. Every minute saved protects brain function.
Transplant
Evaluation, matching, donor readiness, and logistics must align perfectly. Transplant programs rely heavily on coordinators to keep every step synchronised.
Patients searching for the best superspeciality hospital with coordinated care often prioritise these programs. It’s also why many choose Kasturi Medical Centre for their peace of mind.
Tools that make coordination scalable in high-volume Kolkata hospitals
- EMR and shared dashboards: Digital alerts ensure critical results are delivered to doctors immediately.
- Standard checklists: One source of truth prevents confusion.
- Navigation help desks: Patients receive on-the-ground guidance across departments.
Kasturi Medical Centre, a superspeciality hospital in Joka, adopts these systems to manage complexity safely even during peak patient volumes.
How to measure whether coordination is working
Hospitals measure coordination effectiveness through timelines, error reduction indicators, readmission rates, complication tracking, and patient satisfaction metrics.
Better coordination shows measurable results
| KPI | Why It Matters |
| Time-to-diagnosis | Faster decision-making |
| Time-to-treatment start | Reduced disease progression |
| Duplicate test rate | Indicates communication gaps |
| Missed appointment rate | Follow-up discipline |
| Readmissions | Quality of discharge planning |
| Patient satisfaction | Experience indicator |
Kolkata-specific realities
Urban healthcare challenges include cross-department travel, insurance delays, and patients coming from distant regions. Case coordinators bridge these logistical gaps to maintain treatment continuity.
Multiple hospital visits across departments
Patients often move between imaging centres, consultants, and labs across different units. Strong coordination reduces unnecessary back-and-forth and prevents exhaustion.
Insurance delays
Missing documents and pending approvals can stall admissions. Coordinators ensure paperwork and authorisations are completed on time.
Patients travelling from outside the city
Families arriving from smaller towns need planned scheduling. Proper follow-up coordination ensures continuity even after they return home.
Kasturi Medical Centre, a structured superspeciality hospital in Joka, reduces these burdens through organised workflows.
Patient checklist: how to tell if your hospital has strong case coordination
Strong case coordination shows up as clarity, continuity, and accountability, where patients know what’s next, who’s responsible, and how every step connects across their treatment journey
Do I have one point of contact?
A single coordinator or care manager should guide you throughout, ensuring consistent communication and eliminating confusion between multiple teams.
Is there a written next-step plan?
You should receive a clear, documented plan outlining upcoming tests, consultations, and treatments, so nothing is left uncertain or delayed.
Will specialists share notes internally?
All specialists should have access to shared records and be able to update notes in real time, preventing repetition, miscommunication, and fragmented decision-making.
Who tracks follow-ups after discharge?
A defined team or coordinator should actively track follow-ups, appointments, and recovery progress to ensure continuity of care beyond hospital stay.
Crucial Takeaway
Strong case coordination turns complex superspeciality treatment into a clear, organised journey.
When specialists communicate, diagnostics follow the right sequence, and follow-ups are tracked, delays and avoidable risks are reduced significantly. In serious illness, coordination is not supported; it is the foundation of safer outcomes.
Kasturi Medical Centre, a trusted superspeciality hospital in Joka, builds treatment journeys around collaboration, clarity, and patient safety.
Book a consultation.
People Also Ask
Is a case coordinator the same as a nurse?
No. Nurses provide clinical bedside care, while coordinators manage scheduling, communication, documentation, and workflow alignment across departments.
Does coordination reduce treatment cost or just save time?
It does both. Avoiding duplicate tests and delays reduces unnecessary expenses while improving outcomes.
When should families ask for a case coordinator?
Immediately after diagnosis or when multiple specialists become involved in treatment decisions.
What documents should be ready before the first superspeciality consult?
Previous medical reports, imaging scans, medication lists, discharge summaries, biopsy reports, and insurance documents should be organised before consultation.

